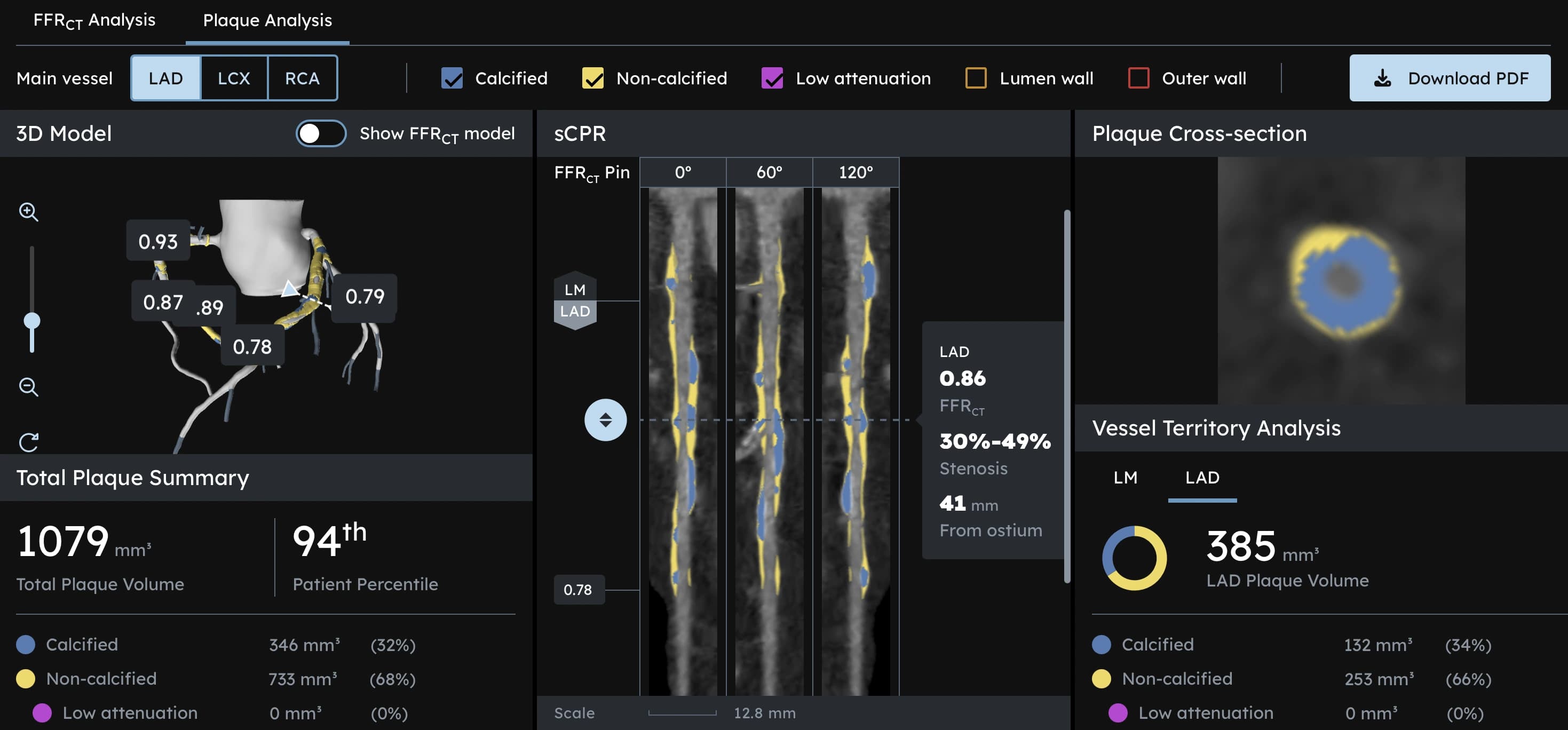
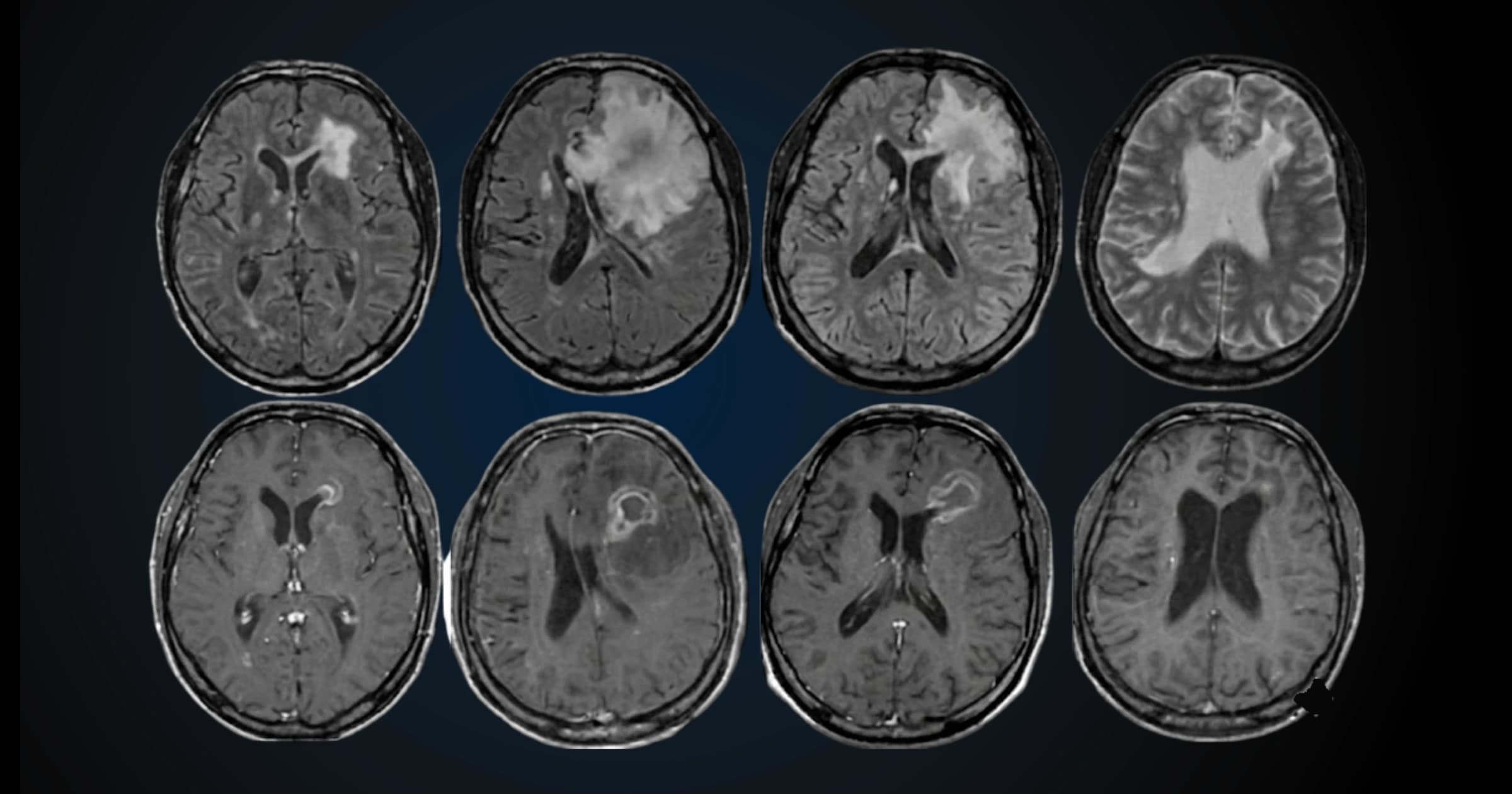
For decades, cardiovascular disease was treated as a plumbing problem: clogged arteries, high cholesterol, poor diet. A landmark 2025 study published in Circulation: Cardiovascular Imaging by researchers at Mass General Brigham has fundamentally reframed that picture.
Analyzing data from 85,551 participants tracked for up to 10 years, the study found that depression and anxiety together raised the risk of major cardiovascular events (heart attack, heart failure, stroke) by approximately 35%, while each condition alone raised risk by about 25%.
The Amygdala Is Not Just About Fear
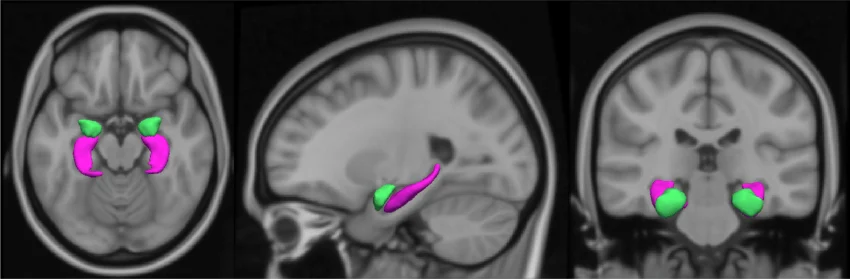
Exhibit 1: T1-weighted MRI scan (axial, sagittal, and coronal view) showing the amygdala in green. Via ResearchGate
The amygdala is a small, almond-shaped structure deep in the brain responsible for processing threat and emotional stress. In people with depression or anxiety, brain imaging shows a measurably higher amygdala-to-cortex activity ratio, meaning the stress alarm fires louder and longer than in people without these conditions.
A 2017 Lancet study, among the first to directly link regional brain activity to cardiovascular outcomes, found that for every one standard deviation increase in amygdala activity, cardiovascular disease risk increased by nearly 60%. The amygdala also signals the bone marrow to produce extra white blood cells, which travel to arterial walls and drive the plaque buildup underlying most heart attacks and strokes.
Three Biological Bridges From Brain to Heart
The Mass General Brigham researchers identified three measurable biological mechanisms linking mental health to heart disease. Together, they form a cascade that connects an emotional state to a physical event.
1. Stress-Related Neural Activity
Elevated amygdala activity directly drives downstream physiological responses, amplifying sympathetic nervous system output. Chronic activation of this stress signaling pathway has been shown to promote atherosclerosis and accelerate cardiometabolic disease.
2. Autonomic Nervous System Dysregulation
Heart rate variability (HRV), the natural beat-to-beat fluctuation of the heart, is a reliable proxy for how well the autonomic nervous system regulates the body. People with depression consistently show lower HRV compared to healthy controls in meta-analyses, reflecting a shift toward overactive sympathetic (“fight or flight”) tone and withdrawn parasympathetic (“rest and digest”) function.
A 2019 study in Frontiers in Psychiatry confirmed that HRV parameters changed measurably with antidepressant treatment, suggesting the cardiac signature of mental illness is both real and reversible.
3. Systemic Inflammation via C-Reactive Protein
C-reactive protein (CRP) is a blood biomarker of systemic inflammation. Depression and anxiety are associated with significantly elevated CRP levels, and high CRP is itself an independent predictor of coronary heart disease risk, even in patients with normal cholesterol.
A large prospective study published in JAMA Psychiatry found that higher CRP levels were associated with increasing risk of hospitalization for depression, suggesting the relationship is bidirectional.
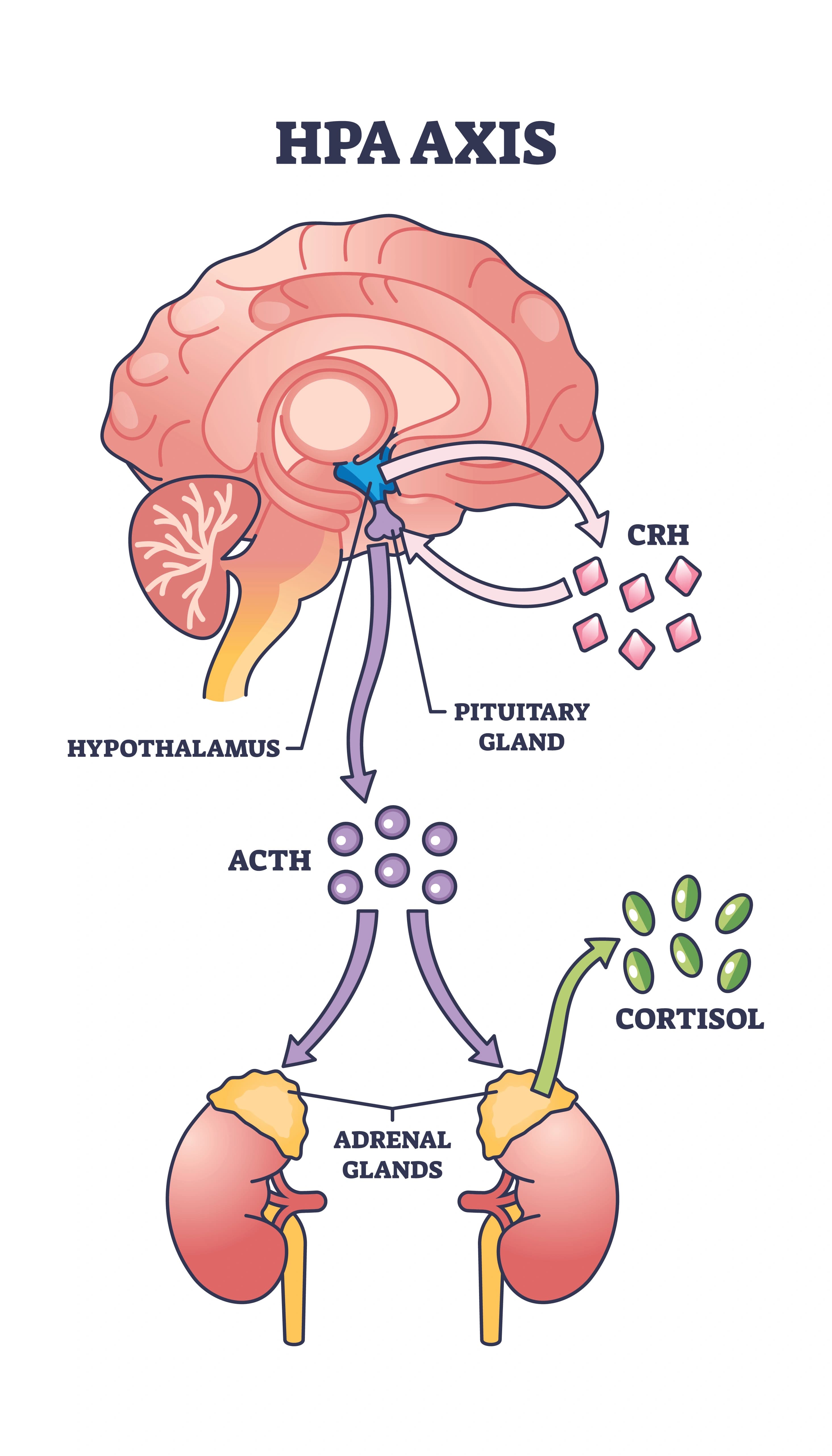
Exhibit 2: Diagram of the HPA (hypothalamic-pituitary-adrenal) axis.
Cortisol: The Hormone That Wears Out Your Arteries
When the stress response fires, the hypothalamic-pituitary-adrenal (HPA) axis releases cortisol.
In the short term, cortisol raises blood pressure, increases cardiac output, and readies the body for action. In the long term, chronic cortisol exposure leads to resistance in its own anti-inflammatory signaling, paradoxically increasing inflammatory cytokines (immunity and inflammation chemical regulators), promoting perivascular inflammation (the accumulation of immune cells around blood vessels), and accelerating coronary artery calcification.
A 2025 study in the European Heart Journal measuring hair cortisol concentrations (a marker of cumulative months-long stress) found that chronic stress levels correlated directly with IL-6 (interleukin-6), an inflammatory mediator, and were significantly associated with acute coronary syndrome. This is not an abstract connection. Stress leaves a biochemical record in your body.
Depression + Anxiety Together Are Worse Than Either Alone
The Mass General Brigham study found that having both depression and anxiety carried roughly a 32–35% greater cardiovascular risk than having either condition alone. This “compounding effect” aligns with what the American College of Cardiology describes as multiple simultaneous pathways, including glucocorticoid (hormones regulating metabolism and suppressing immunity) excess, immune dysregulation, endothelial dysfunction, and health behavior deterioration, all operating in parallel.
An Emory University metareview published in The Lancet Regional Health–Europe in 2025 found that major depression alone raises cardiovascular disease risk by 72%, and more than doubles the mortality rate in people already living with heart disease. Over 40% of people with cardiovascular disease also carry a mental health diagnosis.
What This Looks Like Physically
Mental health conditions are not silent at the tissue level. Sustained amygdala signaling drives arterial inflammation visible on PET/CT imaging. Reduced HRV (Heart Rate Variability, a measure of stress) is detectable on a standard ECG. Elevated CRP (C-reactive protein, liver protein created by somatic stress such as chronic disease) is measurable with a routine blood draw. These are not arbitrary markers; they are the same biomarkers cardiologists already use to predict cardiac events.
Stress activates the sympathetic nervous system and the renin-angiotensin system (a critical hormone system regulating blood pressure, blood volume, and sodium balance), triggering the release of catecholamines and corticosteroids (neurotransmitters) that damage the endothelium (the inner lining of blood vessels) and promote adhesion molecules that recruit inflammatory cells into artery walls. The result is accelerated atherosclerosis (arterial plaque build-up) from the inside out.
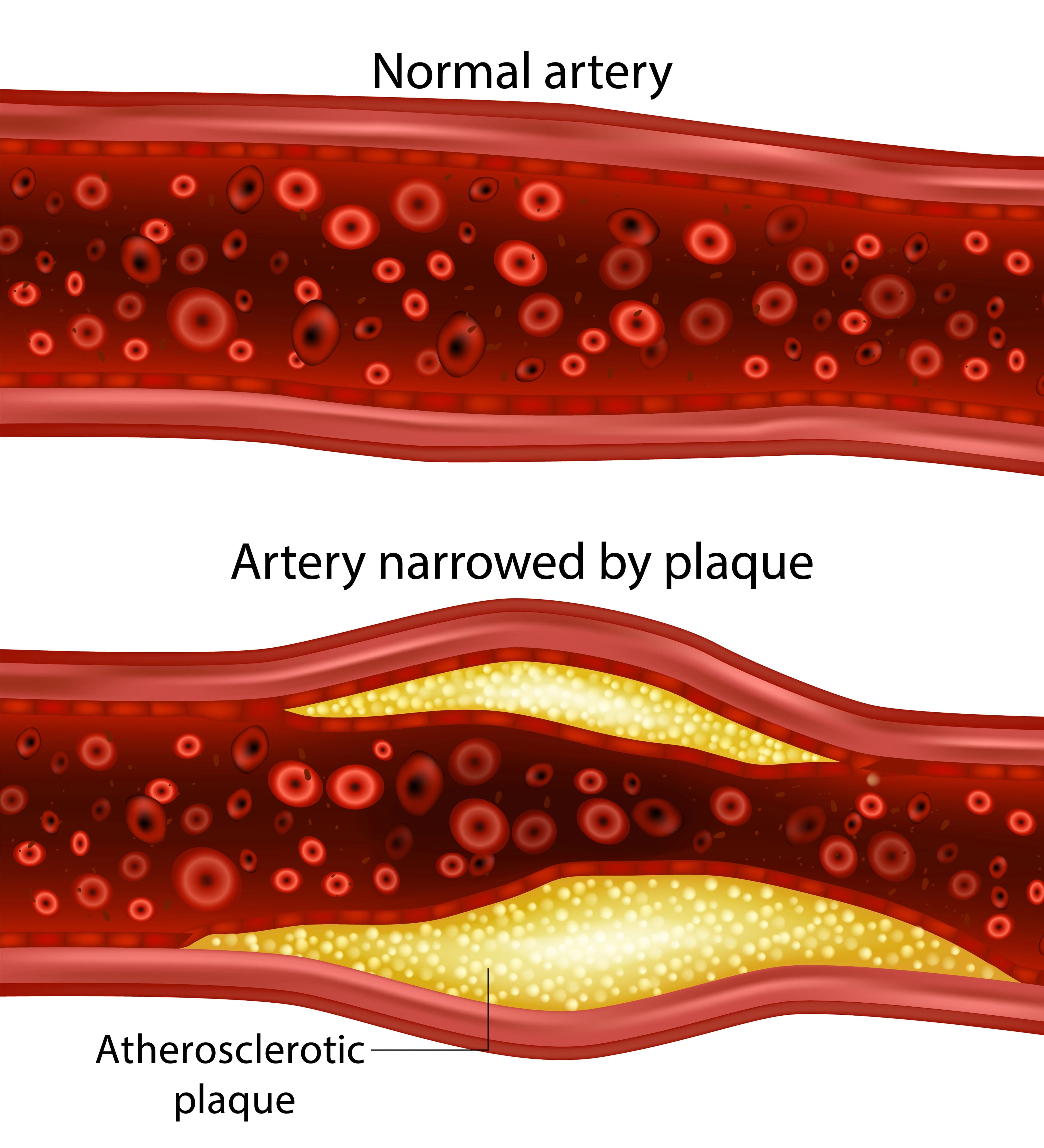
Exhibit 3: A side-by-side comparison of a healthy artery vs. inflamed/calcified artery.
Start Doing Good to Your Body
The good news embedded in this research is that the pathways are modifiable and damage is potentially reversible. Varied treatments today, including lifestyle changes, have already been shown to partially restore HRV toward healthy baselines. And because the mechanism is biological, not just behavioral, addressing mental health is no longer a soft recommendation.
It is a cardiovascular intervention.
Further Reading
1. “Stress May Link Depression and Anxiety to Cardiovascular Disease”. A clinical summary of the Mass General Brigham findings with commentary on therapeutic implications. JAMA
2. “Brain-Body States as a Link Between Cardiovascular and Mental Health”. An emerging framework connecting interoceptive brain-body signaling to both psychiatric and cardiac outcomes. ScienceDirect
3. “Depression and Anxiety Linked to Increased Risk of Heart Attack or Stroke”. An accessible breakdown of the Mass General Brigham study for a general audience. Harvard Gazette
Citations
[1] Abohashem, S., Qamar, I., Grewal, S. S., et al. (2026). Depression and Anxiety Associate With Adverse Cardiovascular Events via Neural, Autonomic, and Inflammatory Pathways. Circulation. Cardiovascular Imaging, 19(1), e017706. link
[2] Tawakol, A., Ishai, A., Takx, R. A., et al. (2017). Relation between resting amygdalar activity and cardiovascular events: a longitudinal and cohort study. Lancet, 389(10071), 834–845. link
[3] Vaccarino, V., Prescott, E., Shah, A., et al. (2025). Mental health disorders and their impact on cardiovascular health disparities. The Lancet Regional Health – Europe, 56, 101373. link
[4] Vaccarino, V., & Bremner, J. D. (2024). Stress and cardiovascular disease: an update. Nature Reviews Cardiology, 21(9), 603–616. link
[5] Black, P. H., & Garbutt, L. D. (2002). Stress, inflammation and cardiovascular disease. Journal of Psychosomatic Research, 52(1), 1–23. link
[6] Hartmann, R., Schmidt, F. M., Sander, C., & Hegerl, U. (2019). Heart Rate Variability as Indicator of Clinical State in Depression. Frontiers in Psychiatry, 9, 735. link
[7] Wium-Andersen, M. K., Ørsted, D. D., Nielsen, S. F., & Nordestgaard, B. G. (2013). Elevated C-Reactive Protein Levels, Psychological Distress, and Depression in 73,131 Individuals. JAMA Psychiatry, 70(2), 176–184. link
[8] Henein, M. Y., Vancheri, S., Longo, G., & Vancheri, F. (2022). The Impact of Mental Stress on Cardiovascular Health—Part II. Journal of Clinical Medicine, 11(15), 4405. link
[9] Wu, Q., Miao, X., Cao, Y., Chi, A., & Xiao, T. (2023). Heart rate variability status at rest in adult depressed patients: a systematic review and meta-analysis. Frontiers in Public Health, 11, 1243213. link
[10] Knezevic, E., Nenic, K., Milanovic, V., & Knezevic, N. N. (2023). The Role of Cortisol in Chronic Stress, Neurodegenerative Diseases, and Psychological Disorders. Cells, 12(23), 2726. link
[11] Magnani, G., Denegri, A., Maccari, C., et al. (2025). The role of chronic psycho-social stress and its link with inflammation in atherosclerotic cardiovascular disease destabilization. European Heart Journal, 46(Supplement_1), ehaf784.3839. link